Why do babies get jaundice?
Jaundice is really common in newborn babies. Approximately 6 in 10 full-term newborns and 8 in 10 preterm babies (born before 37 weeks) will get jaundice.
Babies have more red blood cells when they are born than they need outside the womb. When these red blood cells break down, the byproduct is bilirubin. Because babies have a high turnover of red blood cells, bilirubin can build up in their blood. Usually, our livers process bilirubin, and it is passed out of our bodies in our stools. Because a baby’s liver is immature, it isn’t as effective at removing the bilirubin from their blood, meaning an excess can build up, causing jaundice.
Symptoms of jaundice in babies
Yellow tinge showing:
- On their skin, particularly the face
- In the whites of their eyes*
- Inside their mouth*
- On the palms of their hands and soles of their feet*
You can test for jaundice by placing your baby in bright, natural light to assess their skin tone or by pressing lightly onto their skin.

If your baby has darker skin, it may not be as easy to recognise jaundice from their skin tone. Instead, focus on the other areas of their body mentioned above.
Other symptoms include:
- Baby is sleepy and lethargic
- They may not want to feed as usual
- Have dark yellow urine (should be colourless)
- Have pale poos (they should be creamy yellow or brown)
Contact your midwife or health visitor immediately if your baby has any of these symptoms.
When does jaundice develop?
If your baby is full-term, symptoms usually develop 2 days after birth and get better without treatment within 2 weeks.
If your baby is premature (before 37 weeks), jaundice symptoms may develop within 5-7 days of birth and get better without treatment within 3 weeks.
Breastfed babies are more likely to develop jaundice. This is more common in babies who don’t frequently feed in their first few days (every 1-2 hours) or doesn’t feed very effectively (for example, due to a poor latch).
Jaundice can take a little longer to improve in breastfed babies, although researchers don’t know why this is. If your baby is feeding well and gaining plenty of weight, it will most likely clear up without needing treatment. However, it is worth discussing with your health visitor to rule out any underlying health conditions.
If jaundice develops within 24 hours of birth, it may indicate an underlying health condition or infection. Contact your midwife immediately if this is the case, especially if you are already home.
Postnatal care
As part of the routine newborn physical check-up, your midwife will examine your baby for signs of jaundice within 72 hours of birth. If your baby develops jaundice after this check-up, contact your midwife or health visitor. They will want to check the bilirubin levels and determine if your baby needs treatment or not.
Bilirubin test
If your baby has jaundice, your midwife will check the bilirubin levels to see if they need treatment. This is usually done with a ‘bilirubinometer’. The device shines a light onto your baby’s skin to analyse the bilirubin level. The volume of light reflected or absorbed indicates the level of bilirubin.
In some cases, a blood test may be recommended. For example,
- If the reading from the bilirubinometer is particularly high.
- If your baby develops jaundice within 24 hours of birth.
- If your baby was premature.
Self-treatment
Most babies do not need treatment for jaundice, which will improve within a couple of weeks.
Friends or family may recommend placing your baby in the sunshine to help treat jaundice at home. This is old-fashioned advice and NOT recommended because direct sunlight may cause:
- Overheating: a key risk factor for Sudden Infant Death Syndrome.
- Sunburn. Babies skin is much more fragile than adults and more prone to burning.
Treatment for jaundice
1 in 20 babies will need medical treatment for jaundice due to very high bilirubin levels in the blood. This is because there is a very small chance of the bilirubin passing into the brain and spinal cord and causing damage to the brain and nervous system (Kernicterus).
Babies are more likely to need treatment if they:
- Are premature
- Had a sibling who needed treatment for jaundice
- Are exclusively breastfed
- Develop jaundice within 24 hours of birth
If your baby has any of these risk factors, your midwife or doctor should do an additional check of their bilirubin levels within 48 hours of birth.
If your baby does need treatment, you may be recommended to return to the postnatal ward with them for treatment.
Phototherapy
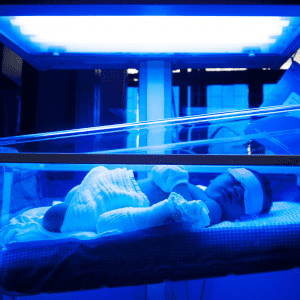
The most common treatment is phototherapy. Baby is placed into a warm incubator or cot with their eyes covered and stripped down to their nappy.
Phototherapy lights are shone onto their skin to help break down the bilirubin. This allows the liver to process the bilirubin more efficiently, and it will pass out in the baby’s stools. You will be encouraged to feed your baby regularly during this treatment, as this can also help them pass more bilirubin in their stools. It will also keep them well-hydrated.
Your midwife will check your baby’s bilirubin levels every 4-6 hours to see how well the treatment is working.
Intensified phototherapy
If they feel the process is not working quickly enough, they may increase the intensity of the phototherapy lights. In this case, a light blanket may be put on your baby alongside the phototherapy lights.
Some babies start with intensified phototherapy if:
- Their bilirubin levels are very high.
- Their bilirubin levels are rising quickly.
Intensified phototherapy treatment cannot be stopped for feeding breaks. In this instance, you would be encouraged to feed your baby expressed breastmilk or formula, usually via a feeding tube. If the baby shows any signs of dehydration, your midwife or doctor may recommend administering IV fluids.
It may take 1-2 days to lower bilirubin levels to safe levels so that treatment can stop and you can return home with your baby. Your baby will need a follow-up blood test 12-18 hours later to check their bilirubin levels remain low.
Other treatments for jaundice
A blood transfusion may be recommended if the baby’s bilirubin levels are very high. This process can take a few hours, and once finished, your baby’s blood will be tested within 2 hours to check the treatment has worked. Sometimes, a baby may need a second blood transfusion if their bilirubin levels remain high. If your baby needs a blood transfusion, it would be in the neonatal unit.
Intravenous immunoglobulin (IVIG) may be recommended if your baby has rhesus disease (when mum is rhesus negative and baby is rhesus positive). This is usually recommended if phototherapy hasn’t worked or their bilirubin levels are rising quickly.
Your midwife or doctor must explain why they recommend one treatment over another so you can make an informed choice on your baby’s behalf. The B.R.A.I.N. decision-making tool can be helpful to use in these discussions.
Breastfeeding and treatment
If breastfeeding and unable to feed your baby on the breast when they are being treated for jaundice, it is essential to pump to maintain your milk supply. This will help you re-establish feeding when the treatment has finished.
The medical team may recommend giving your baby formula within their treatment regime. Tell the team if you don’t want your baby to have formula milk because you want to exclusively breastfeed. They should work with you to create a plan that helps you achieve this. You can also ask your midwife to give you feeding support when your baby is receiving treatment. Especially if your baby has not been feeding effectively or you have any general concerns about feeding.
Other breastfeeding support organisations
The Association of Breastfeeding Mothers
- Helpline: 0300 330 5453
- www.abm.me.uk
The Breastfeeding Network
- The national breastfeeding helpline: 0300 100 0212
- www.breastfeedingnetwork.org.uk
La Leche League
- Helpline: 0845 120 2918
- www.laleche.org.uk
Content Disclaimer
The information contained above is provided for information purposes only. The contents of this article are not intended to amount to advice, and you should not rely on any of the contents of this article. Professional advice should be obtained before taking or refraining from taking any action as a result of the contents of this article. New Life Classes disclaims all liability and responsibility arising from any reliance placed on any of the contents of this article.
References:
NICE [CG98] Jaundice in newborn babies under 28 days. Updated October 2016.https://www.nice.org.uk/guidance/cg98/ifp/chapter/About-this-information
NHS: Newborn jaundice
La Leche League International: Breastfeeding information: Jaundice


